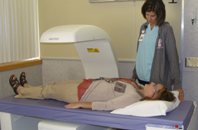
PET/CT Technology at Annie Jeffrey
ANNIE JEFFREY HEALTH CENTER
531 BEEBE STREET
PO BOX 428
OSCEOLA, NE 68651
P: (402) 747-2031
Annie Jeffrey Health Care offers patients a powerful new diagnostic imaging system known as PET/CT. This hybrid technology combines the strengths of two well-established imaging modalities in one imaging session to more accurately diagnose and locate cancers while increasing patient comfort. The service is scheduled to start immediately, in conjunction with Shared Medical Services of Cottage Grove, WI. The PET-CT system will be available as needed in Osceola.
A PET/CT scan is noninvasive and painless. Along with providing better imaging data, it notably increases patient comfort and convenience by reducing the number of scanning sessions a patient must undergo. The procedure is covered by private insurance and Medicare.
PET, or positron emission tomography, monitors the biochemical functioning of cells by detecting how they process certain compounds, such as glucose (sugar). Cancer cells metabolize glucose at a much higher level than normal tissues. By detecting increased glucose use with a high degree of sensitivity, PET identifies cancerous cells - even at an early stage when other modalities may miss them. However, PET cannot pinpoint the exact size and location of tumors to a precision necessary for optimal diagnosis and treatment planning. CT, or computed tomography, yields a detailed picture of the body’s anatomical structures by taking cross-sectional images or X-ray slices of the body. While CT does an excellent job of depicting structures and anatomy, it may miss small or early stage tumors.
Currently, physicians can overlay the results of PET and CT scans performed separately to identify and locate tumors. However, because a patient may not be positioned identically for both scans, the two images can be difficult to line up exactly, degrading the accuracy of the diagnostic information.
The combined PET/CT machine allows physicians to rapidly perform both scans in one session without having to move the patient. This means physicians can precisely overlay the metabolic data of the PET scan and the detailed anatomic data of the CT scan to pinpoint the location and stage of tumors.
Clinical research has shown that in comparison to a PET scan alone, PET/CT technology provides new information that can alter a patient’s treatment plan to better target the cancer in approximately one-third of the cases. In one example, the PET/CT scan of a lung cancer patient revealed not only the original tumor on the lung - which a previous CT scan had found - but an additional tumor the CT missed: a small, early stage lesion in the neck. Based on the CT alone, the physician would have recommended surgery, but the additional tumor found by PET/CT indicated that the cancer had spread and was inoperable. Based on this information, the physician proceeded with radiation therapy, giving the patient a better chance of survival.
While PET/CT is primarily used in cancer treatment, it also has applications in cardiology and brain imaging, and it will help Annie Jeffrey Health Center physicians better understand the workings of heart disease and such neurological disorders as epilepsy and Parkinson’s disease.
For additional information, please call Annie Jeffrey Health Center at 747-2031.
About Us : Medical Staff : Patient Services : Employment : Visitor Info : Foundation : Clinics & Locations : Volunteers : Outpatient Clinics : Home
Privacy Notice : Price Transparency © 2025 Annie Jeffrey Memorial County Health Center. All Rights Reserved. Site created by Midwest Marketing Services.